Seeing redness, bumps, or irritation around your child’s mouth can be unsettling. You may wonder whether it’s just a mild skin reaction or something more serious, like a food allergy. A child mouth rash can appear suddenly, sometimes right after eating, which naturally raises concerns about allergic reactions. The good news is that science gives us clear guidance on how to recognize allergy-related symptoms and how to tell them apart from other common causes. Let’s walk through what research shows, what signs to watch for, and when to seek help.
Understanding Child Mouth Rash
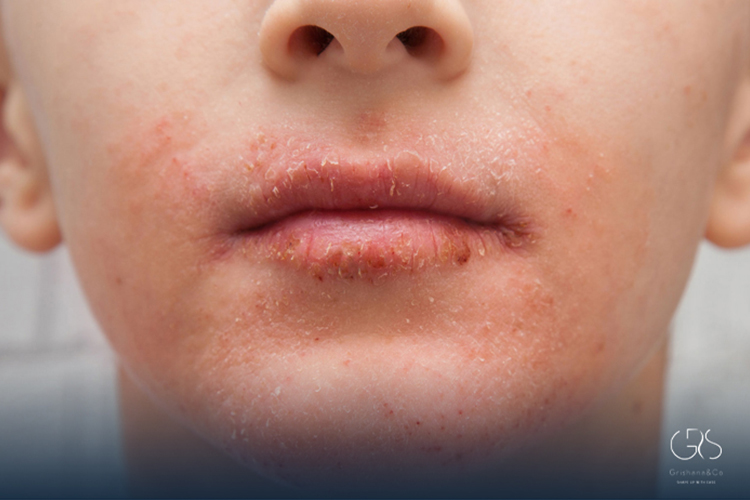
A child mouth rash refers to redness, small bumps, swelling, irritation, or hives around the lips, mouth, or chin area. Sometimes the rash extends slightly onto the cheeks. It may look dry and scaly, or it may resemble hives—raised, itchy welts that appear quickly and fade within hours. The causes vary widely. Some are harmless and temporary. Others require medical attention.
What Does a Child Mouth Rash Look Like?
The appearance depends on the cause. Food-related allergic reactions often cause hives (urticaria), which are raised, itchy patches that can appear within minutes. Contact irritation may cause redness and mild scaling. Perioral dermatitis produces small red papules around the mouth, often sparing the lips themselves. According to the American Academy of Dermatology, perioral dermatitis is common in children and can be mistaken for eczema or allergic rash.
Why the Mouth Area Is Sensitive
The skin around the mouth is thinner and frequently exposed to saliva, food, wiping, and environmental irritants. Repeated exposure weakens the skin barrier. Studies on pediatric dermatology show that saliva and food contact can disrupt the stratum corneum, increasing irritation risk. This makes the area especially reactive—even to non-allergic triggers.

How Food Allergies Cause Child Mouth Rash
Food allergies occur when the immune system mistakenly identifies a food protein as harmful. Immunoglobulin E (IgE) antibodies bind to the allergen and trigger histamine release. Histamine causes itching, redness, swelling, and hives. A child mouth rash from a true IgE-mediated food allergy usually appears quickly—within minutes to two hours after eating.
The Immune System’s Role
Research published in The Journal of Allergy and Clinical Immunology explains that IgE-mediated reactions involve mast cell activation. When histamine is released, blood vessels dilate, leading to redness and swelling. This is why allergy-related rashes often look puffy or hive-like rather than dry and scaly.
Timing of Symptoms After Eating
Timing is one of the strongest clues. If the rash appears consistently within minutes of eating a specific food, suspicion for food allergy increases. The National Institute of Allergy and Infectious Diseases (NIAID) guidelines emphasize rapid onset as a hallmark of IgE-mediated allergy. Delayed rashes hours or days later are less likely to be classic food allergies.
Common Foods Linked to Child Mouth Rash
Certain foods are more commonly associated with allergic reactions in children.
High-Risk Allergenic Foods
The most common triggers include milk, egg, peanut, tree nuts, soy, wheat, fish, and shellfish. According to large epidemiologic studies in the United States and Europe, peanut and tree nut allergies are among the leading causes of severe reactions. A child mouth rash appearing after exposure to these foods deserves medical evaluation.

Acidic and Irritating Foods
Not every rash is an allergy. Citrus fruits, tomatoes, strawberries, and pineapple are acidic and can cause contact irritation, especially in toddlers. This reaction is not immune-mediated. It tends to stay localized around the mouth and does not involve hives elsewhere on the body.
Is It Allergy or Contact Irritation?
Distinguishing between allergy and irritation is essential.
Signs Suggesting a True Allergy
• Hives that spread beyond the mouth
• Swelling of lips or eyelids
• Vomiting, coughing, or wheezing
• Symptoms appearing quickly after eating
The American College of Allergy, Asthma & Immunology notes that systemic symptoms point toward IgE-mediated allergy rather than simple irritation.
Signs Suggesting a Non-Allergic Rash
• Rash limited to contact area
• No itching or only mild discomfort
• No breathing or gastrointestinal symptoms
• Gradual improvement without medication
In these cases, the child mouth rash is often due to irritants rather than immune response.
Oral Allergy Syndrome and Child Mouth Rash
Oral Allergy Syndrome (OAS), also called pollen-food allergy syndrome, can cause itching and mild swelling of the lips and mouth.
What Is Oral Allergy Syndrome?
OAS occurs when proteins in raw fruits or vegetables resemble pollen allergens. The immune system reacts locally in the mouth. Studies show this condition is more common in older children and adolescents with seasonal allergies.
How It Differs from Severe Food Allergy
OAS symptoms are typically mild and confined to the mouth. Severe reactions are rare but possible. Cooking the food often eliminates symptoms because heat denatures the proteins.
When a Child Mouth Rash Signals Something Serious
Most mouth-area rashes are mild. However, some signs require urgent care.
Warning Signs of Anaphylaxis
Anaphylaxis is a severe, life-threatening allergic reaction. Symptoms include:
• Difficulty breathing
• Swelling of tongue or throat
• Persistent vomiting
• Drop in blood pressure
Research confirms that early use of epinephrine significantly reduces complications. Immediate emergency care is essential.
Swelling Beyond the Skin
If the rash is accompanied by facial swelling or hoarseness, seek medical help. These may signal airway involvement.
Diagnosis and Testing for Food-Related Child Mouth Rash
If food allergy is suspected, proper evaluation is crucial.
Skin Prick Testing and Blood Tests
Allergists may perform skin prick testing or measure serum-specific IgE levels. According to NIAID guidelines, these tests help identify sensitization but must be interpreted alongside clinical history.
Oral Food Challenges
The gold standard for diagnosis is a supervised oral food challenge. Studies show this method provides definitive answers when history and tests are unclear.
Managing and Preventing Child Mouth Rash
Prevention depends on the cause.
Avoidance and Label Reading
For confirmed allergies, strict avoidance is necessary. Parents should read ingredient labels carefully. The U.S. Food Allergen Labeling and Consumer Protection Act mandates clear labeling of major allergens.
Protecting Sensitive Skin
If irritation is the issue, gently clean the skin after meals and apply a protective barrier ointment. Dermatology research supports barrier creams to reduce contact dermatitis risk.
When to See a Specialist
If episodes recur or worsen, consult a pediatric allergist. Recurrent child mouth rash with other symptoms should not be ignored.
Supporting Your Child Emotionally
Health concerns can create anxiety for both child and parent.
Talking to Your Child About Food Reactions
Use simple language. Explain that certain foods may not agree with their body. Reassurance reduces fear.
Creating a Safe Eating Environment
Inform caregivers and teachers about confirmed allergies. Having an action plan builds confidence and safety.
Conclusion
A child mouth rash can have many causes, from simple contact irritation to true food allergy. Timing, associated symptoms, and recurrence patterns provide essential clues. Rapid-onset hives, swelling, or breathing difficulty after eating strongly suggest an allergic reaction and require medical evaluation. Localized redness after acidic foods is more likely irritation. Scientific evidence emphasizes careful assessment rather than assumptions. If you’re unsure, consult a pediatrician or allergist for guidance. With accurate diagnosis and thoughtful management, most children with mouth-area rashes can eat safely and thrive confidently.
Sources
- JACI, Guidelines for the Diagnosis and Management of Food Allergy in the United States: Report of the NIAID-Sponsored Expert Panel
- American College of Allergy, Asthma & Immunology, Food Allergy
- American Academy of Dermatology Association, Red rash around your mouth could be perioral dermatitis
- National Institute of Allergy and Infectious Diseases, Diagnosing Food Allergy