If you deal with sneezing fits, itchy eyes, sinus pressure, or relentless postnasal drip, you’ve probably wondered: is daily allergy medication actually safe? For many people with seasonal or perennial allergies, symptoms aren’t occasional they’re constant. That makes daily allergy medication feel less like a choice and more like survival. But is long-term use supported by science? Let’s look at what research, clinical guidelines, and allergy specialists say about safety, effectiveness, and potential risks.
Why People Consider Daily Allergy Medication
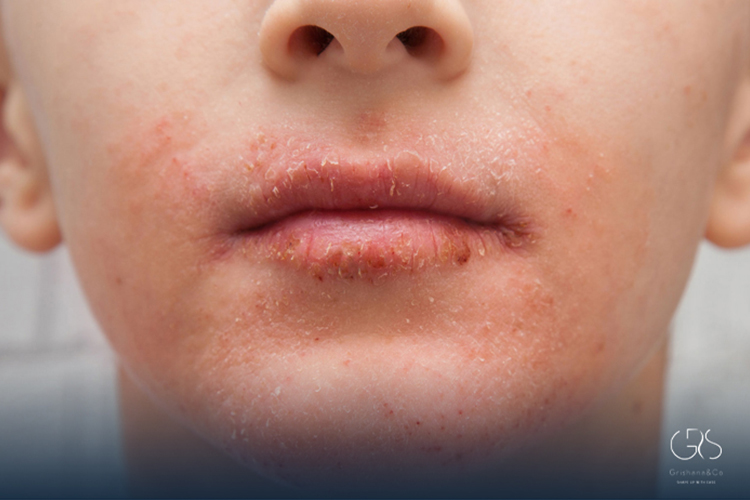
Allergic rhinitis affects up to 30% of adults and 40% of children worldwide, according to the World Allergy Organization. For many, symptoms last months or even all year. Dust mites, pet dander, mold, and pollen don’t take breaks.
Seasonal vs. Perennial Allergies
Seasonal allergies symptoms are commonly triggered by airborne pollens and tend to flare up during the spring or fall months. In contrast, perennial allergies occur throughout the year and are usually caused by indoor allergens such as dust mites, pet dander, or mold. Individuals who experience year-round triggers are more likely to depend on daily allergy medication to keep their symptoms consistently under control.

Chronic Symptoms and Quality of Life
Studies published in The Journal of Allergy and Clinical Immunology show untreated allergic rhinitis significantly reduces sleep quality, cognitive performance, and workplace productivity. When symptoms are persistent, daily treatment may improve overall functioning and well-being.
How Daily Allergy Medication Works
Most daily allergy medication falls into one of three categories: antihistamines, intranasal corticosteroids, or leukotriene receptor antagonists. Each works differently in the immune cascade.
Antihistamines
Second-generation antihistamines such as cetirizine, loratadine, and fexofenadine block histamine receptors without crossing the blood–brain barrier as easily as older drugs. Research confirms they cause significantly less sedation than first-generation antihistamines like diphenhydramine.

Intranasal Corticosteroids
Fluticasone, mometasone, and budesonide reduce inflammation directly in nasal tissue. According to multiple randomized controlled trials, intranasal steroids are the most effective monotherapy for moderate to severe allergic rhinitis.
Leukotriene Modifiers
Montelukast blocks inflammatory leukotrienes. It is sometimes used when antihistamines alone are insufficient, though the FDA has issued warnings regarding potential neuropsychiatric side effects.
Is Daily Allergy Medication Safe for Long-Term Use?
The short answer: for most healthy adults, yes—when used appropriately. Clinical guidelines from the American Academy of Allergy, Asthma & Immunology (AAAAI) support regular use of second-generation antihistamines and intranasal corticosteroids for chronic allergic rhinitis.

Safety of Second-Generation Antihistamines
Large safety reviews show that long-term use of cetirizine, loratadine, and fexofenadine has minimal cardiovascular or neurological risk in healthy individuals. Unlike older antihistamines, they do not significantly impair cognition or reaction time.
Nasal Steroids and Systemic Absorption
One common fear is steroid exposure. However, modern intranasal corticosteroids have very low systemic bioavailability. Studies measuring cortisol levels show minimal suppression when used at recommended doses. This makes daily allergy medication using nasal steroids generally safe for prolonged periods.
What About Children?
Pediatric studies demonstrate that recommended doses of intranasal steroids do not significantly affect growth when monitored. Still, pediatricians recommend regular evaluation to ensure appropriate dosing.
Potential Risks of Taking Daily Allergy Medication
Even though daily allergy medication is generally safe, no medication is entirely risk-free. Awareness helps you use it wisely.
Drowsiness and Cognitive Effects
While second-generation antihistamines are less sedating, cetirizine may still cause mild drowsiness in some individuals. This varies by metabolism and sensitivity.
Anticholinergic Burden
Older first-generation antihistamines have been associated with increased dementia risk when used chronically, according to observational studies in JAMA Internal Medicine. This risk does not appear significant with newer antihistamines.
Tolerance and Effectiveness
Some patients report reduced effectiveness over time, but controlled studies show true pharmacologic tolerance is uncommon. Often, symptom variation reflects allergen exposure changes rather than medication failure.
Benefits of Daily Allergy Medication
When symptoms are persistent, daily allergy medication offers more than comfort—it prevents complications.
Reduced Risk of Sinus Infections
Chronic nasal inflammation can block sinus drainage. Studies show that consistent anti-inflammatory treatment reduces the incidence of secondary sinus infections.
Better Sleep Quality
Allergic rhinitis is strongly linked to sleep-disordered breathing. Treating inflammation daily improves sleep efficiency and reduces daytime fatigue.
Improved Asthma Control
Allergic rhinitis and asthma frequently coexist. Research indicates that controlling nasal inflammation improves asthma outcomes, supporting integrated management strategies.
Who Should Be Cautious?
Although daily allergy medication is safe for most, certain populations require closer supervision.
People with Glaucoma or Urinary Retention
Older antihistamines can worsen these conditions due to anticholinergic effects. Second-generation agents are preferred.
Individuals with Liver or Kidney Disease
Since antihistamines are metabolized or excreted through these organs, dosage adjustments may be necessary.
Pregnant or Breastfeeding Individuals
Loratadine and cetirizine are generally considered low risk during pregnancy, but medical consultation is essential before daily use.
When to Consider Alternatives
If you rely heavily on daily allergy medication but still experience symptoms, you may need a broader strategy.
Allergen Avoidance
Environmental control measures—HEPA filters, dust mite covers, humidity reduction—can significantly reduce symptom burden.
Immunotherapy
Allergy shots or sublingual tablets gradually retrain the immune system. According to long-term studies, immunotherapy can reduce symptoms even after treatment ends.
Biologic Therapies
For severe allergic disease, biologics such as omalizumab target IgE directly. These are typically reserved for complicated cases.
Practical Tips for Safe Daily Use
If you choose daily allergy medication, a few simple habits can maximize safety.
Use the Lowest Effective Dose
More is not better. Follow evidence-based dosing recommendations.
Reassess Periodically
Work with a healthcare provider annually to confirm ongoing need and adjust therapy if necessary.
Monitor Side Effects
Report persistent drowsiness, mood changes, or unusual symptoms promptly.
What Science Ultimately Says
Extensive clinical research supports the safety and effectiveness of daily allergy medication for most individuals with persistent allergic rhinitis. Modern antihistamines and intranasal corticosteroids have favorable safety profiles when used at recommended doses. The key is selecting the right medication type, using it correctly, and reviewing your treatment plan periodically.
For many people, daily allergy medication is not a shortcut—it’s a medically supported strategy to control chronic inflammation, protect sleep, reduce asthma flares, and improve quality of life. Like any long-term therapy, it should be intentional and informed.
Conclusion
So, is it safe to take daily allergy medication every day? For the vast majority of healthy adults and children, scientific evidence says yes,when using modern second-generation antihistamines or properly dosed nasal corticosteroids under appropriate guidance. The benefits often outweigh the risks, especially when allergies are persistent and impact daily functioning. If you’re unsure about your specific situation, a personalized discussion with a healthcare provider can help you create a safe, effective long-term plan.
Sources
- JACI, Intranasal antihistamines and corticosteroids in allergic rhinitis: A systematic review and meta-analysis
- ScienceDirect, Evidence-based use of antihistamines for treatment of allergic conditions
- PubMed Central, Pharmacology, particle deposition and drug administration techniques of intranasal corticosteroids for treating allergic rhinitis